ORIGINAL RESEARCH |
https://doi.org/10.5005/jp-journals-10040-1257 |
Medial Plantar Artery Flap for Heel Reconstruction: A 22-year Follow-up
1,2Department of Plastic Surgery, Lok Nayak Hospital, New Delhi, India
Corresponding Author: Vaishali Srivastava, Department of Plastic Surgery, Lok Nayak Hospital, New Delhi, India, Phone: +91 9312517770, e-mail: wishy22@gmail.com
Received on: 10 April 2022; Accepted on: 09 June 2022; Published on: 31 December 2022
ABSTRACT
Introduction: Heel reconstruction is a surgical challenge because of unique nature of its tissue. The instep flap based on the medial plantar artery neurovascular bundle provides a sensate flap with tissue similar to that of the heel.
Materials and methods: The study includes 29 patients with soft tissue defects of the heel who presented between 1998 and 2021. Medial plantar artery flap was done to cover the defect. The patients were followed up for sensations and any ulceration in the flap for a maximum period of 22 years.
Results: Twenty-nine patients with soft tissue defects of the heel underwent medial plantar artery flap and were included in the study. Eleven patients continued their follow-up for 22 years. All except one flap survived and did not develop any ulceration in long-term follow-up also. Protective sensations were present in the flap in patients who had normal sensations in the foot before surgery. Results were inferior in patients who had decreased sensations in the sole before surgery such as diabetics and postspinal injury patients.
Conclusion: Medial plantar artery flap is a robust and reliable option for heel reconstruction even in long-term follow-up.
Clinical significance: Medial plantar artery flap can be safely opted for heel reconstruction and satisfactory results can be expected even after 20 years.
How to cite this article: Bhandari PS, Srivastava V. Medial Plantar Artery Flap for Heel Reconstruction: A 22-year Follow-up. J Foot Ankle Surg (Asia-Pacific) 2023;10(1):24-27.
Source of support: Nil
Conflict of interest: None
Keywords: Foot ulcer, Heel defect, Heel pad, Medial planter artery, Posterior heel defect, Surgical technique.
INTRODUCTION
Reconstruction of the heel has been a challenging surgery over the course of history due to unique nature of its tissue. The skin is thick with a glabrous epidermis and dermis and beneath it lies a subcutaneous fat layer that is divided into compartments by vertical fibrous septa that extend from periosteum of the calcaneum to the plantar fascia.1 This skin is well adapted to bear the entire weight of the body and withstand pressure forces.2 There is very little laxity to allow primary closure, thus making it imperative to replace it with “like” tissue. The ideal replacement would be the tissue that is durable, sensate, and can withstand the weight of body and shearing forces of walking and other activities like jumping, running, etc., without giving in and yet has low donor site morbidity.3
Various options have been used for reconstructing the plantar surface of foot such as skin grafting,4 muscle flap with skin graft, myocutaneous flap,5 and local fasciocutaneous flaps such as transposition, rotation, V-Y flap,6 reverse sural flap,7 and free flap.8 Since the heel is a weight-bearing area, a skin graft, or in fact any tissue besides plantar area is unable to withstand this stress. Local and free flaps continue to be explored for an ideal option.
The instep forms a part of nonweight-bearing surface on the plantar skin. It provides similar tissue without causing any functional deficit. The instep flap or medial plantar artery flap was first described by Harrison and Morgan in 1981.9 It can be used to cover defects of the lateral sole and heel, and also the lower tendo-Achilles area.10
The instep flap is a robust flap based on the medial plantar neurovascular bundle. The medial plantar artery is the smaller branch of posterior tibial artery which divides at posterior edge of sustentaculum tali. It passes under the abductor hallucis muscle and distally lies between it and flexor digitorum brevis. The lateral edge of abductor hallucis which corresponds to the medial edge of the plantar aponeurosis marks the line along which the perforators emerge to supply the overlying skin. Surface anatomy can be marked as a line drawn between the center of the heel posteriorly extending to the medial sesamoid of the great toe. The medial edge of the plantar aponeurosis can be made prominent by passively dorsiflexing the great toe, which puts the medial part of the plantar aponeurosis under tension. The flap is centered over this line.9,11 Flaps with dimensions of up to 10 cm length × 7 cm width can be raised easily. It has been used as a pedicled as well as a free flap for defects of the heel and forefoot.12 It also has the advantage of being sensate.
The current study presents a long-term follow-up of medial plantar artery flap done for reconstruction of the soft tissue defects of the heel. It aims to ascertain the durability of the flap as it bears the weight and stress over the years.
MATERIALS AND METHODS
The study was conducted at a tertiary healthcare center from 1998 to 2021. Inclusion criteria were patients above 18 years of age with soft tissue defects of the heel following trauma, neurological deficit after spinal injury, malignancy, and diabetic foot.
Exclusion criteria were poor diabetic control and those with previous surgery for the same defect.
Surgical Technique
Preoperative evaluation was done using hand-held Doppler and course of the medial plantar artery was marked. Under tourniquet control, the wound was debrided as necessary. Osteomyelitic bone in patients with diabetes, spinal surgery, and leprosy was also thoroughly debrided. The flap is then marked over the instep area keeping the neurovascular pedicle in midline. The flap elevation was started from the distal marking. The medial plantar artery and nerve were found between the abductor hallucis and the flexor digitorum brevis muscles. The flap was then raised subfascially, under loupe magnification fascicles from the medial plantar nerve supplying the flap were dissected off the nerve and were taken with the flap to make it sensate (Fig. 1). The flap was then transposed onto the defect, the donor site was grafted with split skin graft. A tie-over dressing was done over the grafted area. This dressing was opened and all sutures were removed at 2 weeks. Patient was allowed to ambulate at 4 weeks, initially with support and then without.
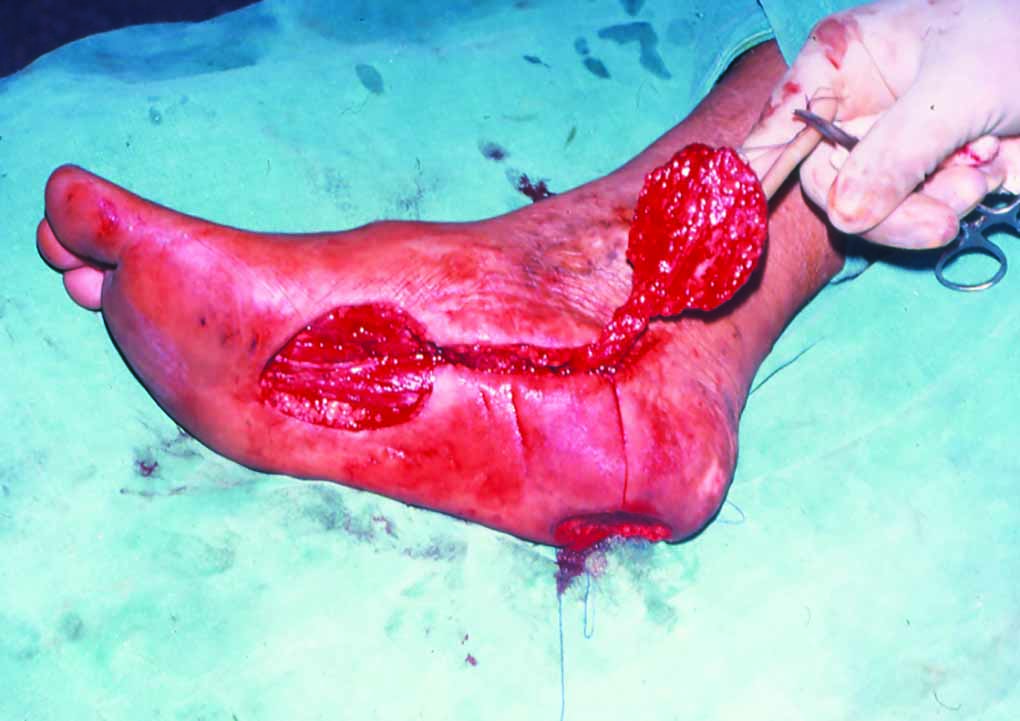
Fig. 1: Medial plantar artery flap: operative photograph
All patients were advised silastic soles for protection during weight-bearing at least for 1 year.
Patient was called for follow-up at 3 months, then at 6 months for next 3 years, and then annually. Patients were asked to report immediately if they develop any ulceration, pain at the operative site, or any other complaint regarding operation. Flap was assessed for any improvement in sensation and ulceration. Crude touch was assessed using a cotton wisp.
RESULTS
Twenty-nine patients with soft tissue defects of the heel were included in the study. There were 18 males and 11 females. Mean age was 27.5 years. Eighteen patients had post-traumatic heel defect, five patients developed soft tissue defect after neuropathy following spinal surgery, two cases were malignant, and four were diabetic foot.
Medial plantar artery flap was successfully performed in all patients. Average flap size was 8.34 × 5.88 cm. Ipsilateral donor site was available in all cases, hence no free flap was done.13 Three patients developed venous congestion in the postoperative period which resolved after removal of few sutures.
Eleven continued their follow-up for 22 years. Eight followed up for more than 10 years, seven for 5–10 years, and three for less than 5 years.
Out of 29 patients, five did not use silastic sole as a protective cover for heel. All these five patients incidentally were farmers and worked barefoot in the field and still did not develop any ulceration over the heel area resurfaced by instep island flap. It was noted, however, that all five of them were operated for a post-traumatic defect of the heel and had no underlying osteomyelitis or sensory deficit.
One patient with heel defect postspinal surgery, underwent thorough debridement of the osteomyelitic calcaneum followed by instep flap for cover. One and half months later he developed a small raw area with purulent discharge on the margin of the wound which was debrided and dressed. The wound healed, however, he did not follow up during the coronavirus pandemic time and eventually came with complete loss of the flap 2 years later.
Rest of the 28 flaps were able to bear weight after 4 weeks and did not develop any ulceration or raw area. Patients with diabetes, leprosy, and postspinal surgery heel defects stayed in regular follow-up for their medical condition and simultaneously with us also. Stringent care and precautions prevented complications in these patients.
Sensations over the flap improved with time and patients were able to appreciate crude touch in 2–3 months which improved over the next 2 years. Results were inferior in patients with already decreased sensation of the foot such as diabetics and those with neurological deficit. They were following instructions to take care of the heel area strictly.
Donor area healed uneventfully with a split skin graft in all patients. However, two patients developed junctional hyperkeratosis along the graft margin.
DISCUSSION
In our study there was flap loss in one patient, survival rate was 96.55%, and there were few minor complications in four patients (13.7%) which were eventually resolved. We encountered no donor site complications. These results were comparable to a review study by Opoku-Agyeman which reports very high flap survival rate (98.2%), low minor flap complications (9.4%), and low donor site complications (5.2%).14
In a study by Schwarz and Negrini,10 the authors reported a 25% complication rate such as infection, delayed healing, pressure sore, and flap necrosis. We report a lower complication rate (13%). All patients in quoted study had ulcers following trauma secondary to sensory loss and the mean age was 50 years. In our study, majority of the patients had post-traumatic defects with intact nerve supply and the mean age was 27.5 years.
Rashid et al.15 compared medial plantar artery flap with sural artery flap for heel reconstruction. They found that though medial plantar artery flap took longer surgical time, it was associated with earlier weight-bearing and lesser complications than sural artery flap. Patients also returned to work sooner, at 8 weeks as compared to 12 weeks with sural artery flap. This is possible as instep skin is glabrous and more akin to the heel skin as compared to any other flap.
Our study reports loss of one instep island flap following osteomyelitis of the underlying bone, Benito-Ruiz et al. also reported loss of one instep flap out of their six patients.16 This was seen in a previously irradiated limb due to which healing was poor. Their study also concluded that the instep flap is an ideal locoregional flap for anterior heel defects.
Oh et al. performed versatile instep flaps in 20 patients.17 Proximally based, distally based, and free flaps were done in 20 patients. They reported partial loss of three pedicled flaps and hyperkeratosis in one patient. Our study reported only loss of one flap and two patients had hyperkeratosis along the graft margin.
Siddiqi et al. published a case series of instep island flap over 14 years.18 They also found it to be a reliable option giving good contour of the heel. The skin texture was well-matched with minimum donor site morbidity. We also observed similar results in our study.
Macedo et al. operated on 12 patients with post-traumatic heel defect.19 They performed medial plantar artery flap to cover defects on anterior calcaneal region, posterior calcaneal region, and dorsum of foot. One patient showed loss of graft on donor site and one patient had partial loss of flap. In all other cases the result was esthetically and functionally acceptable.
Our study shows that instep flap is a good alternative not only in short follow-up period but over a long span of 22 years which validates various studies on this flap.
CONCLUSION
Medial plantar artery flap or instep flap is an excellent flap for heel reconstruction. Even after 22 years the flap is reliable with no ulceration on weight-bearing and has protective sensations. The donor site morbidity is also minimum, making it a superior option to other flaps.
Clinical Significance
Medial plantar artery can be safely used for heel reconstruction with good results in long-term follow-up.
Case 1
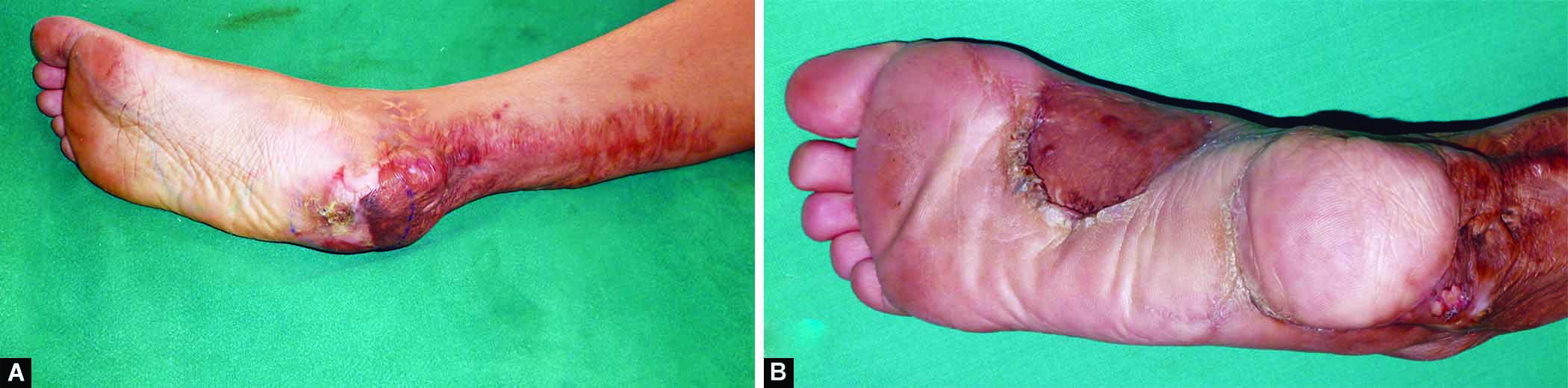
A 25-year-old female patient, presented with a post-traumatic heel defect for 2 months. Sensations of the foot were intact preoperatively. She underwent debridement of the wound. There was no osteomyelitis. Instep island flap was done to cover the soft tissue defect of the heel. Patient was a farmer by occupation, she started working barefoot in the fields within 6 months of surgery. There was no ulceration or raw area on the flap (Fig. 2).

Figs 2A to C: A 25-year-old female patient with a post-traumatic heel defect of size 6 × 6 cm in the right foot. (A) Preoperative; (B) At 1 year; (C) At 22 years
Case 2
A 42-year-old farmer, presented with a post-traumatic soft tissue defect of the heel for 3 months. He was taken for wound debridement along with removal of dead bone. There was no underlying osteomyelitis and sensations of the foot were intact. Instep island flap was used to cover the wound. Patient was able to start weight-bearing at 6 weeks and was working in field at the end of 6 months. The flap was healthy on all subsequent visits. The contour was observed to look like patient’s natural heel over a period of time (Fig. 3).
Figs 3A and B: A 42-year-old farmer with a post-traumatic heel defect of size 8 × 7 cm of the right foot. (A) Preoperative; (B) At 20 years, note the marginal hyperkeratosis around the graft
Case 3
A 61-year-old patient, presented with soft tissue defect of the heel following spinal surgery. Sensations of the foot were diminished. Underlying osteomyelitic bone was debrided thoroughly and wash was given. Instep island flap was used for covering the defect. Flap healed and patient was discharged after suture removal. One and half months later he developed a small area with purulent discharge, wound was curetted and dressed, antibiotics given. The wound settled, however, during the coronavirus pandemic patient could not come for follow-up. He came 2 years later, giving history he had again developed a discharging sinus. He took treatment at a local hospital in his town. After 2 years there was complete loss of the flap (Fig. 4).
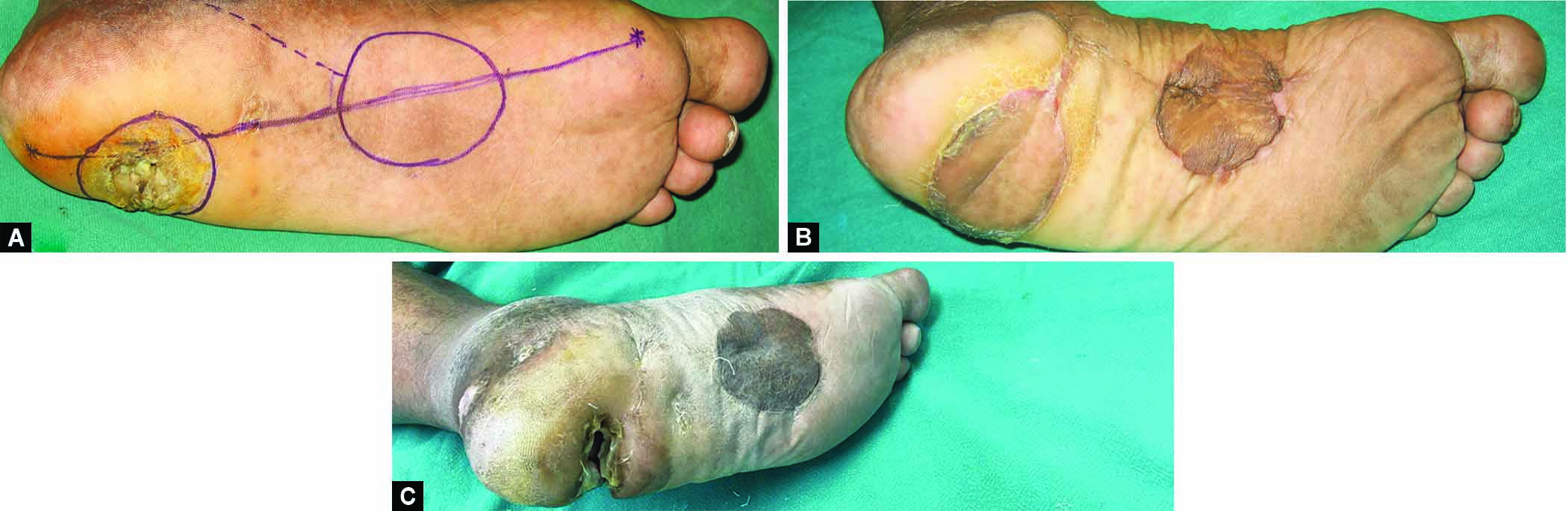
Figs 4A to C: A 61-year-old male patient with heel defect of size 5 × 4 cm following spinal surgery. (A) Preoperative; (B) At 2 months, small area of ulceration at posterior margin of the flap; (C) Complete loss of flap at 2 years
INSTITUTIONAL REVIEW BOARD
The authors did not seek IRB approval for this study because we did not employ the use of protected health information in this investigation.
REFERENCES
1. Roblin P, Healy CM. Heel reconstruction with a medial plantar V-Y flap. Plast Reconstr Surg 2007;119(3):927–932. DOI: 10.1097/01.prs.0000242484.54997.9e
2. Wang M, Xu Y, Wang J, et al. Surgical management of plantar melanoma: a retrospective study in one center. J Foot Ankle Surg 2018;57(4):689–693. DOI: 10.1053/j.jfas.2017.12.004
3. Reiffel RS, McCarthy JG. Coverage of heel and sole defects: a new subfascial arterialized flap. Plast Reconstr Surg 1980;66(2):250–260. DOI: 10.1097/00006534-198008000-00014
4. Singh K, Kundu ZS, Singh B, et al. Heel defect reconstruction using local vascularized flaps: results and clinical outcomes in 16 patients. J Foot Ankle Surg (Asia-Pacific) 2018;4(3):16–20. DOI: 10.5005/jp-journals-10040-1083
5. Saltz R, Hochberg J, Givens KS. Muscle and musclecutaneous flaps of the foot. Clin Plast Surg 1991;18(3):627–638. DOI: 10.1016/S0094-1298(20)30860-9
6. Masquelet AC, Romana MC, Wolf G. Skin island flaps supplied by vascular axis of the sensitive superficial nerves: anatomic study and clinical experience in the leg. Plast Reconstr Surg 1992;89(6):1115–1121. DOI: 10.1097/00006534-199206000-00018
7. El-Shazly M, Yassin O, Kamal A, et al. Soft tissue defects of the heel: a surgical reconstruction algorithm based on a retrospective cohort study. J Foot Ankle Surg 2008;47(2):145–152. DOI: 10.1053/j.jfas.2007.12.010
8. Ring A, Kirchhoff P, Goertz O, et al. Reconstruction of soft-tissue defects at the foot and ankle after oncological resection. Front Surg 2016;3:15. DOI: 10.3389/fsurg.2016.00015
9. Harrison DH, Morgan DG. The instep island flap to resurface plantar defects. Br J Plast Surg 1981;34(3):315–318. DOI: 10.1016/0007-1226(81)90019-9
10. Schwarz RJ, Negrini JF. Medial plantar artery island flap for heel reconstruction. Ann Plast Surg 2006;57(6):658–661. DOI: 10.1097/01.sap.0000235426.53175.e3
11. Cormack GC, Lamberty BGH. Medial Plantar Artery. The Arterial Anatomy of Skin Flaps. 2nd ed. New York: Churchill Livingstone; 1994. p. 373–376.
12. Mourougayan V. Medial plantar artery (instep flap) flap. Ann Plast Surg 2006;56(2):160–163. DOI: 10.1097/01.sap.0000190830.71132.b8
13. Löfstrand JG, Lin CH. Reconstruction of defects in the weight-bearing plantar area using the innervated free medial plantar (instep) flap. Ann Plast Surg 2018;80(3):245–251. DOI: 10.1097/SAP.0000000000001274
14. Opoku-Agyeman JL, Allen A, Humenansky K. The use of local medial plantar artery flap for heel reconstruction: a systematic review. Cureus 2020;12(8):e9880. DOI: 10.7759/cureus.9880
15. Rashid M, Hussain SS, Illahi I. A comparison of two fasciocutaneous flaps in the reconstruction of the weight-bearing heel. J Coll Physicians Surg Pak 2003;13(4):216–218. DOI: 04.2003/jcpsp.216218
16. Benito-Ruiz J, Yoon T, Guisantes-Pintos E, et al. Reconstruction of soft-tissue defects of the heel with local fasciocutaneous flaps. Ann Plast Surg 2004;52(4):380–384. DOI: 10.1097/01.sap.0000105520.24063.bb
17. Oh SJ, Moon M, Cha J, et al. Weight-bearing plantar reconstruction using versatile medial plantar sensate flap. J Plast Reconstr Aesthet Surg 2011;64(2):248–254. DOI: 10.1016/j.bjps.2010.04.013
18. Siddiqi MA, Hafeez K, Cheema TA, et al. The medial plantar artery flap: a series of cases over 14 years. J Foot Ankle Surg 2012;51(6):790–794. DOI: 10.1053/j.jfas.2012.06.003
19. Macedo JLS, Rosa SC, Filho Neto AVR, et al. The medial plantar flap: a case series. Rev Bras Cir Plást 2017;32(2):256–261. DOI: 10.5935/2177-1235.2017RBCP0041
________________________
© The Author(s). 2023 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.